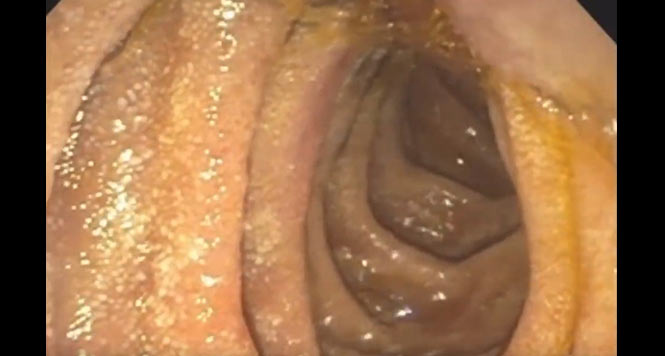
Papillary Morphology Predicts Difficult Biliary Cannulation
Rajesh N. Keswani, MD, MS, reviewing Angsuwatcharakon P, et al. Surg Endosc 2023 Apr 13.
Successful and safe ERCP requires the endoscopist to cannulate the duct of interest successfully and efficiently. Although operator skill clearly influences procedure success, there is growing evidence that the morphology of the major papilla also influences technical success.
There are a few classification systems for major papilla morphology, but they share many similarities. In this study, the classification is described as follows: type 1 has a major papilla diameter >3 mm (ie, regular papilla); type 2 has a major papilla diameter ≤3 mm (ie, small papilla); type 3 has bulging or protruding papilla (ie, papilla that is protruding or bulging into the duodenal lumen, sometimes hanging down, pendulous with the orifice oriented caudally); and type 4 has ridged papilla (ie, the ductal mucosa seems to extend distally out of the orifice, either on a ridge or in a crease) (Gastrointest Endosc. 2019;90:957-963). In prior studies, small and pendulous papillae were associated with difficult cannulation (Surg Endosc. 2021;35:6455-6465).
In this study, 805 naive papillae were retrospectively reviewed in a blinded fashion (to the procedural outcome) and classified into the above system. The authors identified that small papillae (type 2) and creased papillae (type 4) were morphology types associated with difficult cannulation requiring advanced cannulation techniques (eg, double guidewire or precut sphincterotomy). The authors also suggest that the double guidewire technique may be less successful when failing to cannulate a patient with a type 3 morphology.

COMMENTThis study adds to the literature that papillary morphology significantly impacts ERCP difficulty. Although there is some variability in the literature, nearly all studies suggest that “regular” papillary morphology is not associated with difficult cannulation, but that small papillary morphology is associated with difficult cannulation. This study also suggests, with very limited evidence, that the bulging/pendulous papilla (type 3) might be best suited for precut sphincterotomy (rather than the double-guidewire technique) when cannulation is unsuccessful.
Note to readers: At the time we reviewed this paper, its publisher noted that it was not in final form and that subsequent changes might be made.
CITATION(S)
Angsuwatcharakon P, Thongsuwan C, Ridtitid W, et al. Morphology of the major duodenal papilla for the selection of advanced cannulation techniques in difficult biliary cannulation. Surg Endosc 2023 Apr 13. (Epub ahead of print) (https://doi.org/10.1007/s00464-023-10058-1)