Sequenzen:
 Lead-in
Lead-in
Various access routes are available for drainage in patients with cholestasis. In the complex case presented here, neither ERCP nor an attempt at PTCD placement had been successful. Transgastric placement of a metal stent was therefore carried out, leading to rapid decongestion of the bile ducts.
 Sequence 1 — 65-year-old patient with increasing cholestasis
Sequence 1 — 65-year-old patient with increasing cholestasis
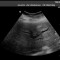
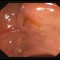
A 65-year-old patient presented with increasing cholestasis and a metastatic gallbladder carcinoma. Ultrasound shows predominantly left-sided cholestasis, with interruption of the common hepatic duct (CHD). An initial attempt at ERCP shows a macroscopically unremarkable papilla. However, it is not possible to probe the bile ducts due to the extensive CHD stenosis. Following papillotomy, a large amount of blood was released across the papilla. The bleeding was self-limiting.
 Sequence 2 — endosonographic transgastric puncture of the bile ducts
Sequence 2 — endosonographic transgastric puncture of the bile ducts
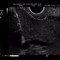
To achieve the urgently needed bile duct relief, an endosonographic access route was now chosen. A previous attempt to place a PTCD for external bile duct drainage had failed, with the CHD still not passable. With endosonographic guidance, transgastric puncture of the S2 branch is carried out using a 19A needle. Wire probing for transpapillary drainage is again unsuccessful. A ductal system dilated to 8 mm is seen, with contrast stopping at the level of the hilum. A more stable transgastric tract is now therefore created using the ring knife and then gradually dilated to a diameter of 10 mm using bougies.
 Sequence 3 — transgastric bile duct relief using a metal stent
Sequence 3 — transgastric bile duct relief using a metal stent
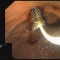
A fully covered metal stent 6 cm long with a diameter of 6 mm is introduced and released via the access route created with the ring knife. A large amount of bile is discharged into the stomach via the stent immediately after the stent release. The final radiographic check shows that the metal stent is in the correct transgastric position. The patient benefited from the intervention in terms of both clinical findings and laboratory tests. The diagram shows the course of bilirubin values before and after .


