Endoscopic diagnosis of celiac disease
Alexander Hann, Benjamin M Walter and Alexander Meining - Ulm
Celiac disease is a chronic inflammation trigged by the ingestion of gluten and resulting in a dense infiltration of lymphocytes in the proximal small intestine. Classic pathological findings in histology are mucosal inflammation, crypt hyperplasia and villous atrophy.
Traditionally celiac disease is diagnosed using duodenal biopsies in combination with serum autoantibodies (1). Since the improvement of video endoscopes that are used in daily practice including the introduction of narrow band imaging (NBI) and near focus, detailed examination of the duodenal mucosa results in an accurate method for the optical diagnosis (2–4). Endoscopically visible hallmarks of celiac disease are scalloped duodenal folds, grooves and fissurations (Table 1). This contrasts with healthy tissue, which is covered with finger-like villi that provide a large surface area for nutrient uptake. In celiac disease, the villi are typically much shorter and less pronounced than they are in healthy mucosa. Under endoscopy, the villous pattern can be further enhanced by the instillation of water and this approach has been regularly used in the assessment of diseases of both the duodenum and the jejunum. Water-immersion is simple, comprising the removal of air from the duodenal lumen followed by the injection of 90-150 ml of water. Thereafter, hallmarks of celiac disease such as scalloped duodenal folds, grooves and fissurations can be readily visualized. Thus, this technique enables the diagnosis of areas exhibiting villous damage in the duodenum with high accuracy (5,6). Nevertheless, although this approach acts to reduce the number of biopsies that are required, it is still necessary to confirm a diagnosis using ex vivo histopathological analysis, especially to exclude diseases that can mimic such an appearance (7).
| Normal duodenal mucosa | Celiac disease MARSH 3 | |
|---|---|---|
| Folds | Regular | Loss of folds Visible fissures Nodular appearance (scalloped folds) |
| Villi | Orderly flattened dry Finger-shaped Raised at endoscopic magnification with water immersion technique |
Absent |
Table 1: Endoscopically visible hallmarks of celiac disease in comparison to normal mucosa
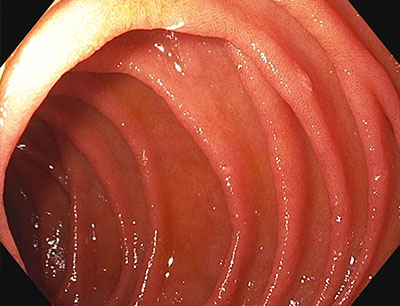
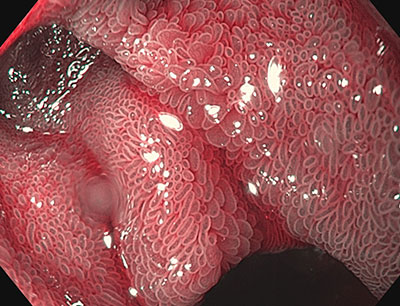
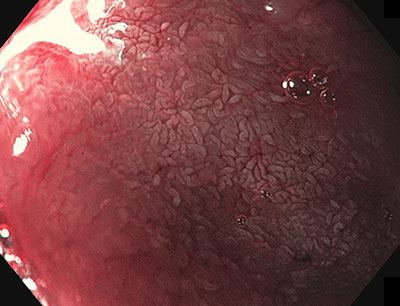
Regular folds and villi
Figure 1: Left image presents regular duodenal folds. The right image presents finger-shaped villi visualized using NBI and near focus.
Figure 2 Left Image presents flattened finger-shaped villi that erect after installation of 100 mL water. Both images were generated using NBI and near focus.
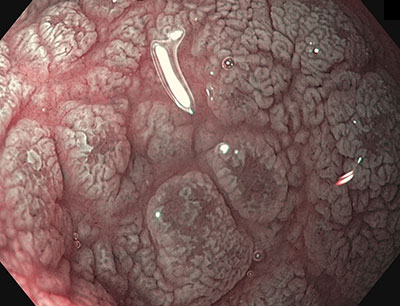
Zöliakie im MARSH-Stadium 3
Figure 3: Left image presents folds with visible fissures and nodular appearance. A closer look at the folds reveals absence of villi. Both images were generated using NBI.
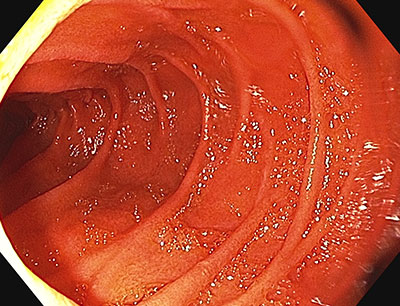
Figure 4: Left image displays loss of folds with a granular appearance of the mucosa. The right image generated using NBI and near focus reveals loss of villi on the mucosal surface.
Figure 5: Left image presents a granular appearance of the folds including visible fissures. The right image generated using NBI and near focus reveals loss of villi.
Improvement after dietary restrictions
Figure 6: Upper left image presenting the initial diagnosis of celiac disease with fissures on the folds and absence of villi when the mucosa was visualized using NBI and near focus in the right image. The lower images were obtained from the same patient after five months of gluten free diet. The lower left image presents regular folds and the right image using NBI and near focus small, but finger-like villi.
References
- Mooney PD, Hadjivassiliou M, Sanders DS. Coeliac disease. BMJ. 3. März 2014;348:g1561.
- Ianiro G, Bibbò S, Pecere S, Gasbarrini A, Cammarota G. Current technologies for the endoscopic assessment of duodenal villous pattern in celiac disease. Comput Biol Med. 1. Oktober 2015;65:308–14.
- Cammarota G, Martino A, Pirozzi GA, Cianci R, Cremonini F, Zuccalà G, u. a. Direct visualization of intestinal villi by high-resolution magnifying upper endoscopy: a validation study. Gastrointest Endosc. November 2004;60(5):732–8.
- Lo A, Guelrud M, Essenfeld H, Bonis P. Classification of villous atrophy with enhanced magnification endoscopy in patients with celiac disease and tropical sprue. Gastrointest Endosc. August 2007;66(2):377–82.
- Hurlstone DP, Sanders DS. High-magnification immersion chromoscopic duodenoscopy permits visualization of patchy atrophy in celiac disease: an opportunity to target biopsies of abnormal mucosa. Gastrointest Endosc. November 2003;58(5):815–6.
- Valitutti F, Oliva S, Iorfida D, Aloi M, Gatti S, Trovato CM, u. a. Narrow band imaging combined with water immersion technique in the diagnosis of celiac disease. Dig Liver Dis Off J Ital Soc Gastroenterol Ital Assoc Study Liver. Dezember 2014;46(12):1099–102.
- Shah VH, Rotterdam H, Kotler DP, Fasano A, Green PH. All that scallops is not celiac disease. Gastrointest Endosc. Juni 2000;51(6):717–20.