Proctology — part 1: diagnosis
D. Wilhelm, L. Calavrezos Array
Chirurgische Klinik and Poliklinik, Klinikum rechts der Isar, Technische Universität München
As a therapeutic discipline, proctology belongs primarily to the field of visceral surgery. However, the diagnosis of proctologic diseases is relevant to all physicians working in endoscopy, who therefore need to ensure that they have the relevant basic knowledge and are able to confidently assess the most frequent clinical pictures. Many proctologic findings may be noted incidentally during routine colonoscopy. However, relevant findings often remain hidden in routine flexible endoscopy examinations, as they can only be adequately assessed using rigid endoscopy.
The aim of this series of articles on proctology is to provide the necessary proctologic information, although limited to the most frequent disease pictures. This first section explains the basic techniques used in a proctologic examination, which — as in any type of clinical picture — provide the basis for successful subsequent treatment.
Basic proctologic diagnosis includes taking a detailed patient history, followed by clinical and machine-aided diagnostic work-up. The latter includes a digital rectal examination and proctoscopy/rectoscopy. Additional examinations are reserved for specific problems and are discussed along with the relevant clinical pictures (Fig. 1).
Taking a detailed proctologic history is essential for establishing a trusting physician–patient relationship, and it is also the most important pillar of diagnosis.
PATIENT HISTORY
Many proctologic diseases show typical clinical findings that can be noted when the patient’s history is being taken and make it much easier to establish the diagnosis. For example, painful conditions, particularly with an acute onset, often affect the highly sensitive anoderm, and a diagnosis of anal fissure is likely if pain first occurs after defecation and has an intense and sharp quality. In addition to allowing the patient to describe the symptoms freely, the history should also include targeted questions on various symptom complexes. These should include the following areas: bleeding and seepage, pain, pruritus ani, and problems with continence or constipation. Taking a detailed and targeted patient history also gives the patient a sense of the physician’s competence and establishes the trust that is decisive for the subsequent clinical examination.
Targeted questions on the following areas should be put when the patient history is being taken: bleeding and seepage, pain, pruritus ani, and problems with continence or constipation.
Bleeding and seepage
Bleeding is always worrying for the patient, as it is associated with cancer and its intensity is usually overestimated. In cases of bleeding, it is decisive to distinguish between acute bleeding (typical of perianal thrombosis, fissures, diverticula and hemorrhoids) and chronic bleeding (inflammatory and neoplastic conditions). However, there is often considerable overlap between the different types of bleeding, and this needs to be taken into account. Light-colored blood is typically found with hemorrhoidal and fissural bleeding, as well as diverticular bleeding, whereas dark, coagulated blood is associated more with chronic inflammatory or neoplastic disease. A distinction also needs to be made between blood deposits on feces (hemorrhoids, ulcer, rectal carcinoma), feces intermingled with blood (colitis, colon carcinoma), and purely peranal bleeding (diverticular bleeding, hemorrhoids). As chronic bleeding is often overlooked as such, clinical signs of anemia should be noted such as a pallid skin color and pale sclerae, as well as poor exercise tolerance. Less worrying, although equally disturbing for the patient, is seepage, which may be evidence of incontinence or may occur with dermatological diseases such as perianal eczema. Seepage is usually associated with pruritus ani (see below) and can be easily identified from moist underwear. A question about soiled underwear should therefore be included as a standard part of a proctologic patient history. More severe problems include mucus secretion, which should always be asked about after cases of rectal and anal prolapse and incontinence; however, a muciparous adenoma may also be present.
Soiled underwear is a sensitive diagnostic tool in relation to seepage, incontinence, peranal bleeding, and pruritus ani.
Pain
As mentioned at the beginning, acute-onset pain indicates problems with the anoderm and in the perianal region, which are among the body’s most sensitive areas. By contrast, rectal diseases usually do not cause any pain, or only mild pain. This aspect is important particularly for distinguishing between perianal venous thromboses and prolapsed hemorrhoidal nodes, which is often difficult for examiners with little proctologic experience. In cases of thrombosis, the patient usually experiences intense pain that only declines slowly over several days, whereas hemorrhoids only cause that type of pain when they are incarcerated and have marked thromboses. Stabbing pain is typical of genital herpes. By contrast, patients feel the most severe pain in cases of fissure, with the pain increasing again at each defecation and leading to a characteristic tension in the sphincter apparatus. A temporal relationship between pain and defecation is therefore important, both in relation to the initial event and also the subsequent course. Chronic increasing pain that is perceived as dull and diffuse (protopathic pain) occurs in cases of abscess and fistula and other inflammatory diseases, but also in anal carcinoma. By contrast, rectal carcinoma is usually asymptomatic, as are numerous dermatological conditions.
Pruritus ani
Perineal itching is often associated with parasitosis (e.g., pinworm eggs of Enterobius vermicularis), but pruritus is usually a nonspecific symptom indicating an overmoist perianal region and excessive contact with irritant agents. The latter may derive from feces (for example, with excess consumption of coffee, citrus fruit and chocolate) and may thus be evidence of occult incontinence (fistulas, hemorrhoids). Alternatively, there may be external factors such as cosmetics, with excess use of moist sanitary wipes and soap, or from clothing. As many patients treat the itching with excessive anal hygiene, this often gives rise to a vicious circle, and patients need to have this explained to them. However, dermatological diseases such as perianal eczema, psoriasis, streptococcal dermatitis, and mycoses are also often associated with pruritus. As patients are often silent about perineal itching, attention should be given during the clinical examination to secondary signs such as traces of scratching.
Incontinence and constipation
While incontinence is primarily a problem in older patients, symptoms of constipation are often diagnosed in middle-aged and also younger patients. Symptoms of incontinence are often only mentioned at more advanced stages (grade 3 incontinence for solid stool), so that targeted questions need to be put about milder forms (disturbance of fine continence, grade 1: incontinence for gases; grade 2: incontinence for liquid stool). The stool consistency should be recorded at the same time, as liquid stool is not perceived in cases of disturbed anorectal sensitivity and can therefore not be checked. In addition to the grade of incontinence, distinctions are made relative to the frequency of occurrence, passive and urge incontinence, and soiling, which is typical of the presence of rectocele. All of these parameters provide information about the severity and possible etiology of the incontinence and should ideally be recorded using a standardized questionnaire, which also allows objective assessment during the subsequent course of treatment. Scoring systems that are often used include the Wexner score (Cleveland Clinic Florida Fecal Incontinence Score) and the Williams score.
Assessing stool consistency is important for constipation as well, in addition to systematic recording of potentially conditioning drugs (e.g., in patients with Parkinson’s disease). In addition to recording stool frequency, increasing attention has recently focused on associated symptoms such as those listed in the Rome classification. Ideally, a scoring system should be used in constipation as well — the Altomare or Longo ODS, or the Cleveland Clinic Constipation Scoring System (CCSS). These include the following parameters, among others: the completeness of defecation and the need to assist it; the frequency of toilet visits and time spent on the toilet; and associated symptoms. Frequent toilet visits may well be connected with constipation here, particularly when defecation is unsuccessful or incomplete, typically in the presence of a defecation disturbance (obstructed defecation syndrome, ODS). By contrast, a low frequency of bowel movements is more often found with transit disturbances, which may also be a sequela of defecation problems. In addition, it should be clarified whether the patient is using laxatives. Both in patients with incontinence and also those with constipation, any previous surgery (particularly proctologic) is important, and in female patients the number and course of births.
In patients with constipation, there is an increasing diagnostic focus on accompanying symptoms and the need for assistance during defecation, in contrast to stool frequency alone, which was previously the decisive parameter.
CLINICAL EXAMINATION
The clinical examination is divided into inspection and digital rectal examination, both of which form obligatory components of a proctologic examination. The clinical examination is the second pillar of proctologic diagnosis. For adequate assessment and identification, familiarity with normal findings and anatomic conditions is relevant, and these will be discussed here initially.
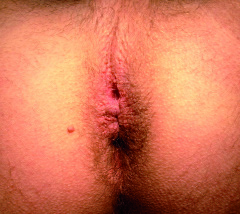
With its fine, radial puckering, the anus is distinct from the surrounding perianal region and also has different coloring, which may be ruddy to bluish. The anus should have a symmetrical shape, and depending on the patient it may be either shallow or funnel-shaped. Even when the patient is relaxed, the anus should have basic tonicity and closure. The epidermal squamous epithelium is dull and at most only slightly reflective in comparison with the perianal region, but it must be distinct from the shiny mucosal surface of the rectum, which becomes visible in rectal prolapse. There should be no fistular orifices and no diffuse reddening (perianal eczema) or localized reddening (abscess) in the perianal region. The anus continues dorsally into the intergluteal cleft and ventrally into the raphe of the scrotum (Fig. 2).
At the start of the examination, the anus should be carefully inspected, with the patient placed in a comfortable position. This is usually a left lateral position, or the lithotomy position if possible. All conspicuous features must be documented with details of their position, with the anal region being described in the same way as positions on a clock face. The ventral side of the anus, toward the symphysis, corresponds to the 12-o’clock position and the side toward the sacrum corresponds to the 6-o’clock position (relative to the situation in the lithotomy position). The examination must be carried out with the necessary care and discretion and the patient should be given understandable comments on it (Fig. 3).
During the inspection of the anal region, all conspicuous features must be documented with details of their position. For this purpose, the anus is described in the same way as positions on a clock face.
Initially, the anal region is inspected, with the buttocks being separated if necessary. Many diseases can already be diagnosed at this stage, such as abscesses, condylomas, rectal prolapse, and perianal venous thrombosis. By contrast, sentinel piles usually only have a low diagnostic value. The anus should show normal closure, with no sign of incontinence — which may be suspected if there is evidence of residual feces or reddening in the perianal region (as a sign of disturbed fine continence).
Dermatological diseases such as anal eczema, mycosis, condyloma, and neoplastic changes in the anoderm (Bowen’s disease) are often single-glance diagnoses. Nodulations of any sort and the presence of scars as evidence of previous surgery are of particular interest. In addition to inspection alone, the patient should be asked to press down and tense the sphincter muscle, as a rough test of the functioning of the sphincter apparatus. It is important here to ensure sufficiently long pressing, as mild forms of rectal prolapse and hemorrhoids may otherwise be overlooked. It should be ensured here once again that the patient is sufficiently relaxed. During pressing, the pelvic floor must descend and the sphincter muscle must relax; this usually also leads to bulging of the anoderm. Conversely, tensing of the anus leads to lifting of the pelvic floor. Basic neurologic tests for orientation supplement the inspection. In what is known as the anocutaneous reflex, sphincter contraction occurs after peranal stimulation. In addition, perianal sensitivity should be tested separately on each side.
Inspection is followed by the digital rectal examination, which should not be limited to assessment of the anal canal alone but should also include assessment of the perianal region (for nodules, indurations, fluctuations, fistular tracts). The digital rectal examination should only be carried out after a careful patient history has been taken, as the history provides diagnostic information that is relevant to the examination and may influence the further procedure. Digital exploration of the anal canal may in some circumstances be more sensitive than visual assessment with the proctoscope or rectoscope, or the diagnostic quality may be much better after a rough digital localization (for fistulas, anal papilla, fissures, anal carcinoma). The digital examination thus has special importance.
The obligatory digital rectal examination is a highly sensitive diagnostic measure, particularly in the anal canal.
One should make sure that sufficient time is available for the digital rectal examination and that it is carried out with appropriate thoroughness. For this purpose, the perianal region and the examining finger should be moistened with an adequate quantity of anesthetic lubricant and the finger should then be slowly introduced into the anal canal. The patient should be asked to press, so that the sphincter is relaxed. The physiological course of the anal canal in the ventral direction should be taken into account. If it has been possible to identify a painful region beforehand (e.g., anal fissure, which is usually located at the 6-o’clock position), then it is best to introduce the finger off center in order to spare the affected area. Alternatively, with painful processes it may only be possible to carry out an adequate investigation after the patient has been sedated. In addition to the assessment of superficial changes in the anal canal, sphincter tone at rest, during pinching, and during pressing should be evaluated again here. If the examiner has sufficient experience, the finger may be able to replace an elaborate manometry examination.
During pressing, particular attention should be given to relaxation of the sphincter tone (the anorectal reflex). This examination is extremely important in patients with obstructed defecation syndrome in particular. The continuity of the sphincter and sphincter length should also be included in the assessment. The location of rectal tumors in the vicinity of the sphincter can be very well assessed digitally, and for this purpose the patient should be asked to tense the sphincter so that it can be identified.
During the rest of the examination, the whole circumference of the rectal ampulla should be palpated. Any rectoceles and intussusceptions that are present can already be noted digitally. Attention should be given to the presence of possible neoplasias and indurations, and it should be pointed out once again that around one-third of rectal carcinomas can be palpated in the digital rectal examination. Attention should also be given here to displaceability relative to the surroundings/bowel wall (Mason classification). Bidigital assessment of the perianal region between the thumb and the intra-anal finger may identify deep abscesses and also fistular tracts. This examination should therefore be added especially in patients with dull, deep pain. By contrast, other types of pathology, such as hemorrhoids, are more accessible to visual and proctologic diagnosis, although they may be felt as a soft cushion. The examination closes with palpation of the prostate or cervix.
PROCTOSCOPY/RECTOSCOPY
A basic proctologic examination ends with proctoscopy or rectoscopy, which should be carried out routinely. However, the two methods have different specific indications, and they are therefore not used as complements. The importance of rigid rectoscopy has declined in recent years. It only continues to be of value in individual areas, such as measuring the distance between rectal tumors and the anocutaneous line, as well as rectoceles and intussusceptions. By contrast, proctoscopy has a unique characteristic in comparison with flexible endoscopy in that it is clearly superior to it for assessing processes in the anal canal. In addition, the preparation process for rigid instruments is much less expensive, and this needs to be taken into account when only anal processes are being assessed. The proctoscope and rectoscope consist of metal sleeves connected to a light source. The rectoscope is much longer (20–25 cm) and can be closed with a gastight seal. The rectoscope provides visualization as far as the distal sigmoid. By contrast, the proctoscope is open and shorter. Due to their rigid structure, both instruments can be used to tense the mucosa of the anal canal and assess it adequately. As the two instruments hold the anal canal open without insufflation, hemorrhoids in particular can be well assessed (Fig. 4).
While rectoscopy is declining in importance, proctoscopy continues to be an indispensable method.
Proctoscopy
Special preparation for proctoscopy is not usually required, but an enema can be administered if appropriate. As mentioned above, proctoscopy should only be carried out after a detailed patient history has been taken and after the digital examination. Patient information should also be provided, despite the low-risk nature of the examination. For the examination, the patient should again be placed in a relaxed position, such as the left lateral or lithotomy positions. The proctoscope is carefully introduced into the anus, with accompanying explanation being given; different sizes of instrument can be used depending on the anatomic conditions. The proctoscope has an internal obturator that provides internal illumination when the light source is withdrawn, and with its conical tip it makes it easier to introduce the proctoscope. The instrument has adequate lubricant applied for introduction and is inserted in alignment with the perineal region in the direction of the navel, with rotation. Here again, it is useful to ask the patient to press in order to relax the sphincters. The previous digital rectal examination also aids the process of introduction, as it already leads to slight dilation and anesthetization of the anal canal. After the sphincter region has been passed (3–5 cm from the anus), the proctoscope/rectoscope has to be tilted sacrally to follow the anatomic course of the rectum (the anorectal flexure). During intubation, it is very important to take sufficient time and explain the precise procedure to the patient.
The proctoscope should also be warmed to a lukewarm temperature, and intubation should not be carried out blindly against resistance. As mentioned above under the digital examination, it may be necessary to sedate the patient, as in cases of fissure. The proctoscope should be introduced as far as the stop ring to ensure complete assessment of the anal canal, even in the presence of funnel anus. The internal obturator is then removed, the cold light source is attached, and the proctoscope is slowly withdrawn with rotatory movements that allow visualization of the entire circumference. Due to its length, the proctoscope is much easier to guide than the rectoscope. Due to the shortness of the instrument, the light yield is also superior. Despite this, it may sometimes be difficult to expose discrete findings, so that locations that were conspicuous during the digital examination need to be assessed with particular care. In addition, it is advisable to separately assess sites of predilection for proctologic diseases (crypt regions, hemorrhoid complexes at the 3-o’clock, 7-o’clock, and 11-o’clock positions, fissures at the 6-o’clock position, etc.). Goodsall’s rule should be noted in relation to the location of potential fistulas. The internal fistular orifices are not necessarily located in the crypt region and may also occur in the distal rectum. If necessary, the examination can be supported with the use of probes and dye solutions that are introduced into the external fistular orifices. Indirect signs should also be noted, such as hypertrophic anal papillae and sentinel piles (skin tags) as signs of chronic fissure. Depending on the situation, it may be advantageous to expose the anal canal using cotton applicators or tweezers.
The importance of purulent secretion and thickened crypts should be mentioned. Before the proctoscope is withdrawn through the anal canal, the patient should be asked to press, so that any rectoceles present or internal rectal prolapse can be verified. At the level of the hemorrhoid complex, the patient should be asked to press again, so that hemorrhoidal prolapse can be assessed. By contrast, hemorrhoids should be assessed at rest without provocation. Suitable instruments for rubber-band ligation of hemorrhoids are easily introduced through the proctoscope, and hemostasis and injection are also easily carried out.
The proctoscope is used to assess the anal canal, diagnose and treat hemorrhoids, and to clarify fistulas and fissures.
Rectoscopy
Intubation with the rectoscope is carried out in the same way, also with an obturator in place. However, the rectoscope should not be introduced to the maximum extent at once; the obturator should first be exchanged for a magnifying cap after the anal canal has been passed. This gives the rectoscope an airtight seal, so that further intubation can be carried out with visualization. Advancing the endoscope also allows for air insufflation with a balloon, enabling the rectum to be expanded. With visualization and illumination via the attached optical fiber, the rectoscope can be advanced around the rectal fold structures as far as the lower sigmoid. In contrast to proctoscopy, preparation with an enema is therefore advisable. Particularly with the option of air insufflation, rectoscopy is suitable for diagnosing rectoceles and rectal ulcers, but inflammatory and neoplastic changes can also be extremely well assessed and confirmed with biopsies. Special large biopsy forceps are used for the purpose. Hemostasis by injection or coagulation can also be carried out rectoscopically. The rectoscope is also particularly well suited for treatment of bleeding in the rectum, which is often intense, as even larger coagula can be suctioned away easily and powerful high-frequency probes as in open surgery can be used. As in proctoscopy, however, areas of interest can also be exposed using pledgets. One disadvantage with proctoscopy and rectoscopy is that it is very difficult to document and demonstrate the findings, as the conventional techniques do not include a video connection.
Rectoscopy is used to assess the rectum and tumors located in it, as well as rectoceles and rectal intussusception.
ADDITIONAL EXAMINATIONS
DThe basic proctologic examination can be supplemented with additional methods, although these are reserved for special issues. Endosonography in particular should be mentioned here, as it extends the range of diagnosis to deeper layers and is still indicated today despite continuing improvements in magnetic resonance technology. In addition, various radiological examinations can be used, such as defecography and transit time assessment. Anal manometry and electrophysiology are indicated particularly for clarifying incontinence, and rarely in patients with obstructive disturbances.
Figure 1
Figure 2
Figure 3
Figure 4
What you need to know
Since the early 2000s, meta-analyses based on smaller studies have shown that open and laparoscopic surgery for rectal carcinoma produce similar results. The most recently published meta-analysis to appear in a major journal — as so often, by a research group in China (1) — included six randomized studies with 1033 patients, including one dating from 2003 with 28 patients (sic!) from a local Brazilian journal published by the University of São Paolo (Rev Hosp Clin Fac Med Univ São Paolo). It is to be hoped that the authors of the meta-analysis read the study as a full publication in the original language. The other studies had been published in English-language journals, but were in some cases so small (with totals of 99–204 cases) that it would need a brilliant statistician to identify any differences that were not gigantic. The only reasonable study, the CLASSIC trial (n = 381) (2) found no difference in the circumferential resection margin, but a slightly lower (HR 0.72) 3-year survival rate, although with an identical disease-free 3-year survival. Overall, the results of the “meta-analysis” for the two procedures are equivalent so far as the statistical analysis is concerned, but the hazard ratio figures suggest that the case numbers are nevertheless not sufficient (2). Another meta-analysis by a Chinese group was published in 2014, this time with 16 studies, most of which could already have been included in the 2011 study (3). So caution needs to be observed with meta-analyses.
A large European study including 1044 patients (the COLOR II Study) was published in April this year, showing equivalent oncological results with the two procedures at the 3-year follow-up in relation to locoregional recurrences, disease-free survival, and overall survival. The case numbers (from 30 hospitals over a 4-year period) are thus similar to those in the six studies included in the meta-analysis described above. However, very advanced tumors (including T4) were excluded, and the boundary used was 15 cm ab ano. Randomization was 2 : 1 for surgery; just under 60% and around one-third of the patients received radiotherapy or chemotherapy preoperatively. Depending on the parameters, follow-up data after 3 years were available for 74–89% of the patients. The study was designed to establish equivalence or noninferiority (4). After 3 years, the results were as follows:
| Laparoscopy | Open | Difference | |
|---|---|---|---|
| Locoregional recurrence | 5.0% | 5.0% | 0 |
| Disease-free survival | 74.8% | 70.8% | 4.0 n.s. |
| Overall survival | 86.7% | 83.6% | 3.1 n.s. |
In both groups, the circumferential resection margin was not tumor-free (defined as a distance of 2 mm) in 10% of cases, and the other data on complete resection were also nearly identical.
Subsequently, two smaller randomized studies from the USA/Canada (n = 489) and from Australia/New Zealand (n = 475) comparing the two procedures have just been published in JAMA. They both report poorer results in the oncological parameters for the laparoscopic variant (no follow-up is available). The North American study (5) from 35 hospitals presented the results for 486 patients who were included, with 462 evaluable patients with rectal carcinomas (up to 12 cm ab ano, no T4) over 5 years — i.e., an average of just under three patients per center and year. This does not mean that inexperienced physicians were involved, but rather that as usual in everyday clinical work, most patients were not included for reasons of time or for other organizational reasons, or did not provide consent (the relevant figures are not given). In addition, the numbers of patients included varied at different centers, and it is also not clear whether all of the hospitals started the study at the same time point. This patient selection, which has to be accepted with almost all multicenter studies, can however in principle mean that the representativeness of the data for all of the relevant patients is at least debatable. The study in Australia and New Zealand (6) used a similar approach, with 475 patients being included at 24 centers over four and a half years (473 were evaluated). T4 tumors were excluded here as well, and as in Europe the rectum was 15 cm long. Neither study offers any follow-up as yet, so that the main outcome parameters were histopathological, consisting of the same composite score based on the distal and circumferential resection margin (> 1 mm), and the quality of the entire mesorectal excision with blinded pathology. Complete resection was noted when all of the end points were reached, either completely or almost completely in North America (i.e., R0 with a margin of less than 1 mm) or completely in Australia. The results were then as follows:
| Composite Outcome | Laparoscopic | Open |
|---|---|---|
| USA/Canada | 92.1% | 95.1% |
| Australia / New Zealand | 82% | 89% |
However, due to the different definitions used, it is worthwhile — at least for a surgeon — to look more closely at the three individual parameters mentioned above. If the 1-mm boundary in both studies is strictly observed, the complete resections achieved were as follows:
| Circumferential resection margin | Laparoscopic | Open |
|---|---|---|
| USA/Canada | 87.9% | 92.3% |
| Australia/New Zealand | 65.8% | 75.3% |
| Europe | 90% | 90% |
| Distal resection margin | Laparoscopic | Open |
|---|---|---|
| USA/Canada | 92.1% | 95.1% |
| Australia/New Zealand | 98.3% | 98.2% |
| Complete total mesorectal excision |
Laparoscopic | Open |
|---|---|---|
| USA/Canada | 92.1% | 95.1% |
| Australia/New Zealand | 87% | 92% |
It can be seen from this that the distal resection margin was not a problem, but the circumferential one certainly was, particularly in the USA (although in both groups). Comparison with the European study, in which only the circumferential resection margin was reported, reveals the differences most clearly.
The contradictory results are not very easy to explain. The NEJM study is larger and uses oncological outcomes instead of surrogate parameters, but follow-up results are lacking. Could it be due to the quality of the surgery? But that was quite well established with minimal numbers and a reviewed video of a procedure before the start of the study; despite that, the European groups perhaps had better expertise. However, the statistics are difficult for laypersons to read; the means for the main outcome parameters (composite score, see above) are within the assumed range of noninferiority in both studies. In the methodology, the studies assumed a range of 6% (North America) to 8% (Australia) for noninferiority. In the composite score, North America reached differences of 3% and Australia 7% — both thus apparently in the normal area, and the P values are also below 0.05. Despite that, the overall range has to be used. In this case, the lower boundary for the actual range of results (lower boundary, 95% confidence interval) in North America was –10.8% (10% was assumed) and in Australia –12.4% (8% was assumed), so that the target was just missed. But when you have to dig deeper into the statistical deliberations in order to understand the results, slight concerns arise. Perhaps both studies were simply not sufficiently powered? In the end, the criticism of the study’s main parameter, which is a surrogate parameter, stands. As the authors themselves mention, the follow-up may show different conclusions — hopefully both studies are sufficiently powered for it. More patience in resisting pressures to publish would therefore be helpful sometimes … From our point of view, the NEJM study will until then continue to be the superior one for evidence, and we would not want to leave unchallenged the warning that laparoscopic surgery should be downgraded. The aim should certainly be to carry out these procedures in specialized centers, so that experience can be better concentrated.